A Novel Analysis to Establish Renal Heterogeneity and Echogenicity Norms in a Healthy Pediatric Population
Wayland J. Wu, MD1, Bradley Morganstern, MD1, Vinaya Vasudevan, MD1, Amanda Myers, BS2, Matthew Elmasri, BS1, Megan Murphy, BS2, Lane S. Palmer, MD1, Sleiman R. Ghorayeb, PhD2
1Division of Pediatric Urology, Cohen Children's Medical Center, New Hyde Park, NY, USA, 2School of Engineering and Applied Sciences, Ultrasound Research Laboratory, Hofstra University, Hempstead, NY, USA.
BACKGROUND: The perceived echogenicity of the newborn kidney appears to change with time relative to the liver and spleen. The characterization of that change has been macroscopic and poorly defined. We previously used a novel approach to assessing renal parenchymal changes on ultrasound of children with congenital ureteropelvic junction obstruction. Herein, we sought to define normal heterogeneity as measured by heterogeneity index (HI) among normal pediatric kidneys and to better elucidate the subtle changes in renal echogenicity seen in children.
METHODS: We identified children whose kidneys were imaged by ultrasound for non-nephrologic, non-urologic disease. Each image was evaluated by a novel program which converts pixels in a gray-scale ultrasound to a binary map to produce HI. From this program, we were also able to objectively analyze echogenicity by calculating the percentage of pixels that were above the 50% mark of the grey scale. When available, we determined the HI and echogenicity of the spleen and liver to establish a ratio with the ipsilateral kidney. Patients were stratified according to age: day of birth, 0-6 months, 6 months-1 year, 1-4 years, 4-12 years, and >12 years. Associations between age and heterogeneity or echogenicity was evaluated by ANOVA, significant findings were analyzed by Tukey-Kramer method.
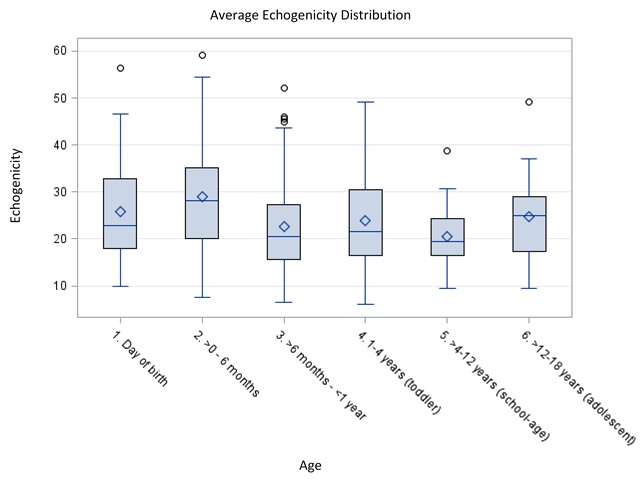
RESULTS: There were 319 renal units available for analysis. Patient age ranged from day of birth to 19 years with 30.4% under 6 months of age. The average HI overall was 1.24 (SD=0.24) without any association with age (p = 0.2561, Fig 1). However, changes in echogenicity was associated with age and was highest up until 6 months old (p = 0.0046, Fig 2). Comparison of echogenicity between the kidney and liver demonstrated that the liver had statistically lower echogenicity than the kidney, in subjects age < 6 months and statistically higher after age 6 months (p = 0.0012). The same was not true when examining the kidney with spleen.
CONCLUSIONS: We establish a standard HI value of normal kidneys in children to be 1.24 providing a reference with which to compare diseased kidneys undergoing US and to provide a non-invasive, non-ionizing method of objectively measuring renal pathologies. Secondly, objective changes to renal parenchymal echogenicity occurs with time with age of 6 months being the critical time point. The change in echogenicity appears to be homogenous as there is no change in overall HI in kidneys based on age. Comparisons of echogenicity between liver and kidney are reliable but not between spleen and kidney.

Back to 2017 Program
