Relative Value Units Do Not Reflect Complexity and Operative Time in Hypospadias Surgery
Kyle A. Gillis, MD, Nicholas H. Chakiryan, MD, David Jiang, MD, Ann Martinez Acevedo, MS, James Christopher Austin, MD, Casey A. Seideman, MD.
Oregon Health and Science University, Portland, OR, USA.
Background
Work relative value units (wRVU) are a value measure assigned by the United States Medicare for reimbursement based on a procedure's operative time, technical skill, effort, and stress. In theory, wRVU accounts for operative time, resulting in equivalent RVU per unit time for short and long procedures. This study aims to assess if operative time and complexity of hypospadias surgery is adequately accounted for in the current RVU system.
Methods
The American College of Surgeons National Surgical Quality Improvement Program Participant User File (ACS-NSQIP PUF) database from 2012-2017 was utilized. Hypospadias current procedural terminology (CPT) codes, including acceptable secondary codes outlined in the AUA Policy & Advocacy Brief. Cases were excluded if concurrent CPT codes were not listed as acceptable secondary codes. The primary variable of wRVU per hour (RVU/hr) was calculated using median total wRVUs and median operative time (excluding anesthesia time). Multivariate linear regression analysis was used to assess factors influencing RVU/hr variable.
Results
10,548 cases were included in the final study population amongst six categories: simple distal (MAGPI, V-Flap), one-stage distal, one-stage mid, one-stage proximal, first stage of two-stage repair, second stage of two-stage repair. Summary shown in Table 1. For one-stage hypospadias operations, simple distal procedures generated the highest median RVU/hr at 15.5; this decreased to 9.8 for proximal procedures. For staged hypospadias, first stage repairs generated a median RVU/hr of 12.2 compared to second stage of 8.0 median RVU/hr.
Student's t-test demonstrated one-stage hypospadias procedures had a higher RVU/hr compared to two-staged procedures (15.9, 95% CI: 15.5-16.2 vs. 9.9, 95% CI 9.2-10.2; p<0.001). Simple distal, distal and midshaft hypospadias had statistically significantly higher RVU/hr compared to proximal hypospadias (single or staged): 16.2, 95% CI: 15.8-16.5 vs. 11.8, 95% CI 10.4-13.1; p<0.001).
Multivariate linear regression revealed that each additional hour of operative time was expected to decrease RVU/hr by 10.1 (-10.1, 95% CI: -9.7 - 10.5, p < 0.001); total work RVU had a statistically significant independent association with RVU/hr (0.59, 95%CI: 0.53 - 0.65, p <0.001).
Conclusion
This analysis of contemporary large population national-level data suggests that the work RVU system significantly favors shorter, less complex procedures in hypospadias surgery. 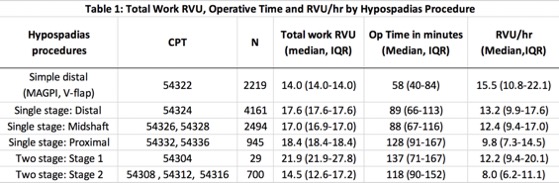


Back to 2019 Abstracts




